 
His LDH decreases to 302 IU/L during his induction phase. 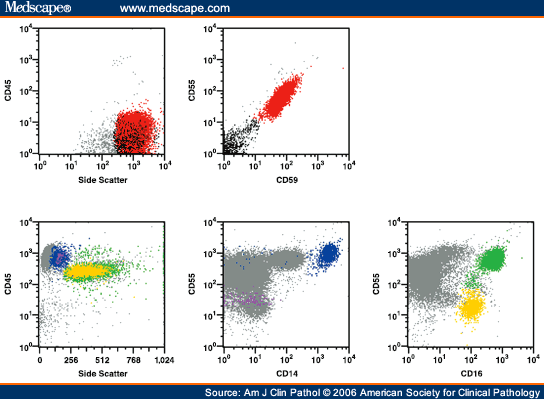
Following induction, he is maintained on eculizumab 900 mg every 2 weeks but continuing to require 1 to 2 units of packed red cells every 4 to 6 weeks. PNH flow cytometry reveals 18% PNH erythrocytes, 85% PNH granulocytes, and 87% PNH monocytes. He had required 6 units of packed red cells in the past month to maintain a hemoglobin greater than 7.5 g/dL. He reports reddish-dark urine in the morning most days of the week, a dull backache, and transient impotence. Complete blood count reveals a hemoglobin of 6.7 g/dL, leukocytes of 3.8 × 10 9/L, platelets of 98 × 10 9/L, and an absolute reticulocyte count of 287 000 mm 3. This 44-year-old man presents with a chief complaint of bright red hemoglobinuria, fatigue, chest pain, dyspnea on exertion, and difficulty swallowing liquids and solids after mowing his lawn on a hot summer day. Patient 2: a 44-year-old man with classical PNH I discontinue anticoagulation if thrombotic symptoms are resolved and the patient is well controlled (LDH <1.5× the upper limit of normal) on a complement inhibitor 30,31 however, discussion with the patient is advised given the paucity of data concerning the risks vs benefit of this recommendation. I usually overlap anticoagulation and complement inhibition for 3 to 6 months as long as there are no other provoking factors. I consider untreated PNH a provoking factor, and do not feel patients with PNH need indefinite anticoagulation however, some hematologists recommend indefinite anticoagulation. 12,13,29 The major advantage is that ravulizumab’s terminal half-life is 4 times that of eculizumab, and it can be administered intravenously every 8 weeks after the 2-week induction phase. It targets the same C5 epitope as eculizumab and has been shown to be noninferior in head-to-head clinical trials. 24 I now consider ravulizumab the treatment of choice for PNH. Eculizumab or ravulizumab should be started as soon as possible to prevent further thrombosis because anticoagulation alone is insufficient for long-term control. Direct oral anticoagulants are likely equivalent but have not been well studied in PNH. Comments about patient 1Īnticoagulation with heparin or low-molecular-weight heparin is still the first action to take in the setting of an acute thrombotic event. Repeat blood counts revealed a hemoglobin level of 9.7 g/dL, 7.0% reticulocytes, and an LDH of 271 IU/L. Her dyspnea and abdominal pain resolved, and her warfarin was discontinued after 3 months of anticoagulation. 
Following the standard eculizumab introduction period (600 mg intravenously, weekly), she was maintained on 900 mg intravenously (biweekly). 
She was vaccinated against Neisseria meningitides and started on eculizumab. PNH flow cytometry revealed an absence of GPI-anchored proteins on 60% of her erythrocytes, 88% of her monocytes, and 94% of her granulocytes, establishing the diagnosis of PNH. She presented with an absolute reticulocyte count of 181 000 mm 3 and a lactate dehydrogenase (LDH) level of 647 IU/L (reference range, 119-226). A complete blood count revealed a leukocyte count of 3.7 × 10 9/L, a hemoglobin of 7.7 g/dL, and a platelet count of 102 × 10 9/L. Intravenous heparin was administered, and she was transitioned to warfarin with a goal international normalized ratio of 2.0 to 3.0. She was on no regular medications and had no family history of thrombosis. Her medical history was unremarkable other than preeclampsia with her second pregnancy. She denied gross hemoglobinuria, difficulty swallowing, or headache. Lower extremity dopplers did not reveal any deep venous thrombi, and a Tech–hepatobiliary iminodiacetic acid scan was normal however, a CT scan of the abdomen revealed hepatic and splenic vein thrombosis with extensive collaterals. An abdominal ultrasound raised the possibility of acalculous cholecystitis, so the patient was admitted to the hospital where a computed tomography (CT) scan was done, revealing a right-sided pulmonary embolism. This 45-year-old woman with no medical history presented with 3 weeks of intermittent, crampy, right upper quadrant abdominal pain, fatigue, dyspnea, and pleuritic chest pain. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |

 RSS Feed
RSS Feed
